As a physical therapist, the words ‘hamstring injury’ will sound immediate alarm bells. It’s a serious situation and for most therapists, it can become very overwhelming very quickly. But today I want to change that.
I spent 13 years in professional sport and private practice dealing with some of the most complex hamstring injuries. At first, I was far from confident. I would throw everything I had at it but struggled to make anything stick.
Like most therapists, I just didn’t have the confidence and clarity to make real changes. I couldn’t achieve those consistent results my patients needed. But something had to change. I couldn’t send elite athletes back without being sure they had the result they needed.
So today, I want to share with you the exact system that I and every one of the ProSport therapists use. I’ll share the inner workings of my system and how it can help you get the results you need even with the most complex of hamstring cases…
A system that over 700 therapists worldwide are already using and seeing immediate rewards.
So, read on to find out;
- The truth about hamstring injuries.
- Testing a hamstring injury.
- A simple hamstring load tolerance test for you to implement immediately.
- A simple guide to your hamstring rehab exercises.
- Using a step-by-step system to get the results you need.
The Hard Truth About Hamstring Injuries
In a 2011 article published on br j sports med, Askling et al stated that hamstring injuries are the single most common injury in elite football. So, if you’re in sports physical therapy then I can guarantee you’re going to see your fair share of hamstring injuries.
But it isn’t just limited to athletic activities. In 2016, Kuske et al highlighted a ‘largely unrecognised population of adults suffering hamstring injuries from low-impact activities.’ The truth is, with the risk factors so widely spread, if you think you’ll get away with not being 100% confident on hamstring strain rehabilitation then you’re going to get a real shock sooner or later.
For me, hamstring strain injuries are serious. I can’t tell you how many I have seen throughout my 13 years in professional sport and private practice. An athlete would come in off the field after that initial injury and the pressure was on.
There would be coaches standing over me asking… ‘Is it bad? Are they going to play tomorrow? Will they fully recover?’ This may have been a less than ideal setting to diagnose and deal with hamstring muscle damage but it gave me the chance to put my system to the test.
So, if you’re a physical therapist and you’re still in the dark or overwhelmed by the thought of rehabbing a hamstring injury then I want to help.
Read on for your complete guide to hamstring rehab…
Testing For Hamstring Muscle Injuries
Before you consider exercises and your rehab process for hamstring injuries we are going to have to cover testing. Most therapists can’t spot a true hamstring strain or hamstring injury from distance. In fact, that would be near impossible.
What every physical therapist needs is a foolproof way of testing so you can understand the true extent of the injury. Without this fundamental set of skills, you can never truly know where you’re going with your rehab. You’re essentially going in blind.
So, how do we test for hamstring strains or tears?
Toe Touch Test
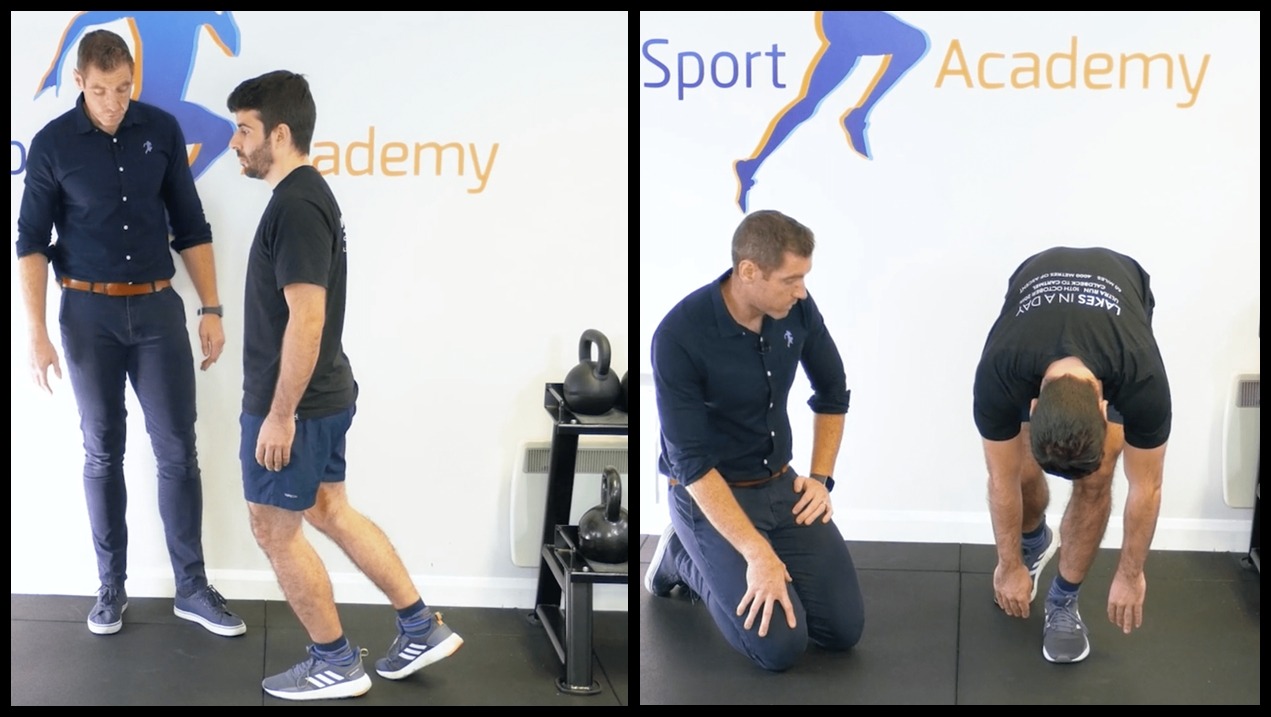
The first place I start when testing a hamstring strain injury is a simple toe touch test. All you’re asking my patient to do is reach down and touch their toes. Every physical therapist has done it 1000 times, right? Well, you don’t want to go simply through the motions. You should be making sense of what you see.
Firstly, if your patient does have a hamstring muscle injury this toe touch test is going to elicit pain in that hamstring muscle group of the affected leg. But it isn’t just pain that you need to pay attention to. You need to look closely at your patient and their movement.
As they reach down you want their weight to shift back but we are also looking at the reaction of the lumbar spine and the ribcage. Could either of those be contributing to their hamstring tightness?
If you do suspect a lack of ribcage mobility could be contributing to the hamstring issue then it will be a case of using breathing techniques or working with the ribcage manually. You want to assist it in going through a full range of motion. Always clear the ribcage first.
However, if your patient is moving well but struggling to keep the knee straight then we could think there is a protective tone around the hamstrings or there could be an issue with the lumbar spine.
In that scenario, we would see if the lumbar tissues are opening up by asking the patient to get into all four positions and looking for that protective tone. If there is an issue with the low back you will see a flattening of the lumbar tissue.
Proximal Knee Flexion
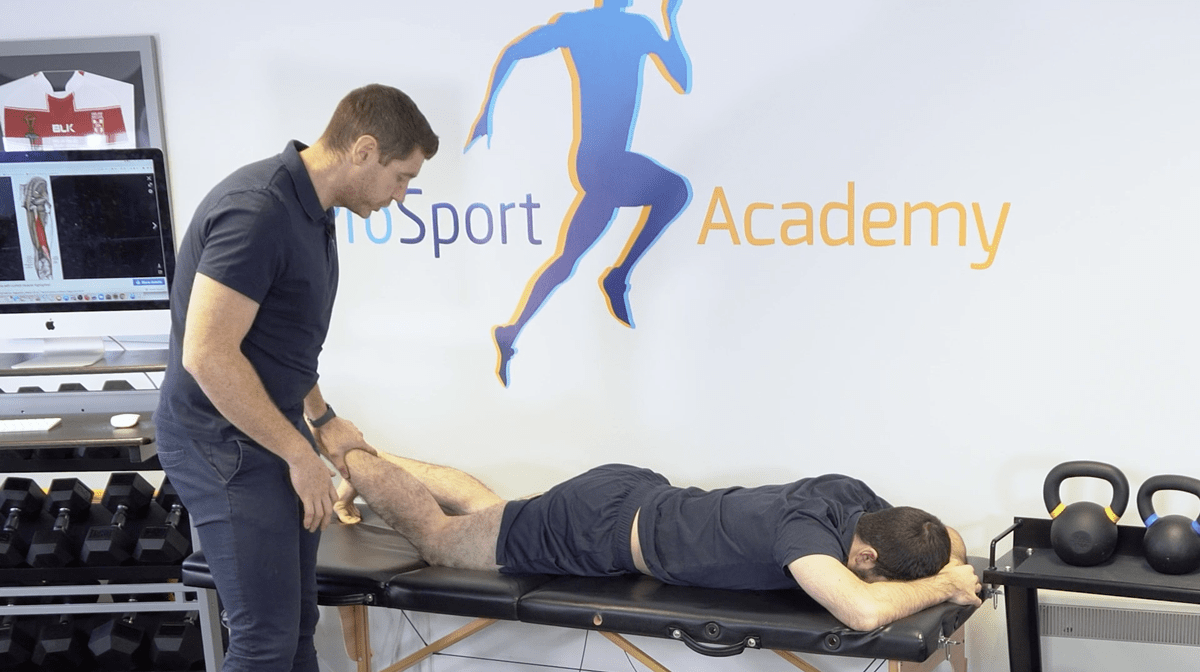
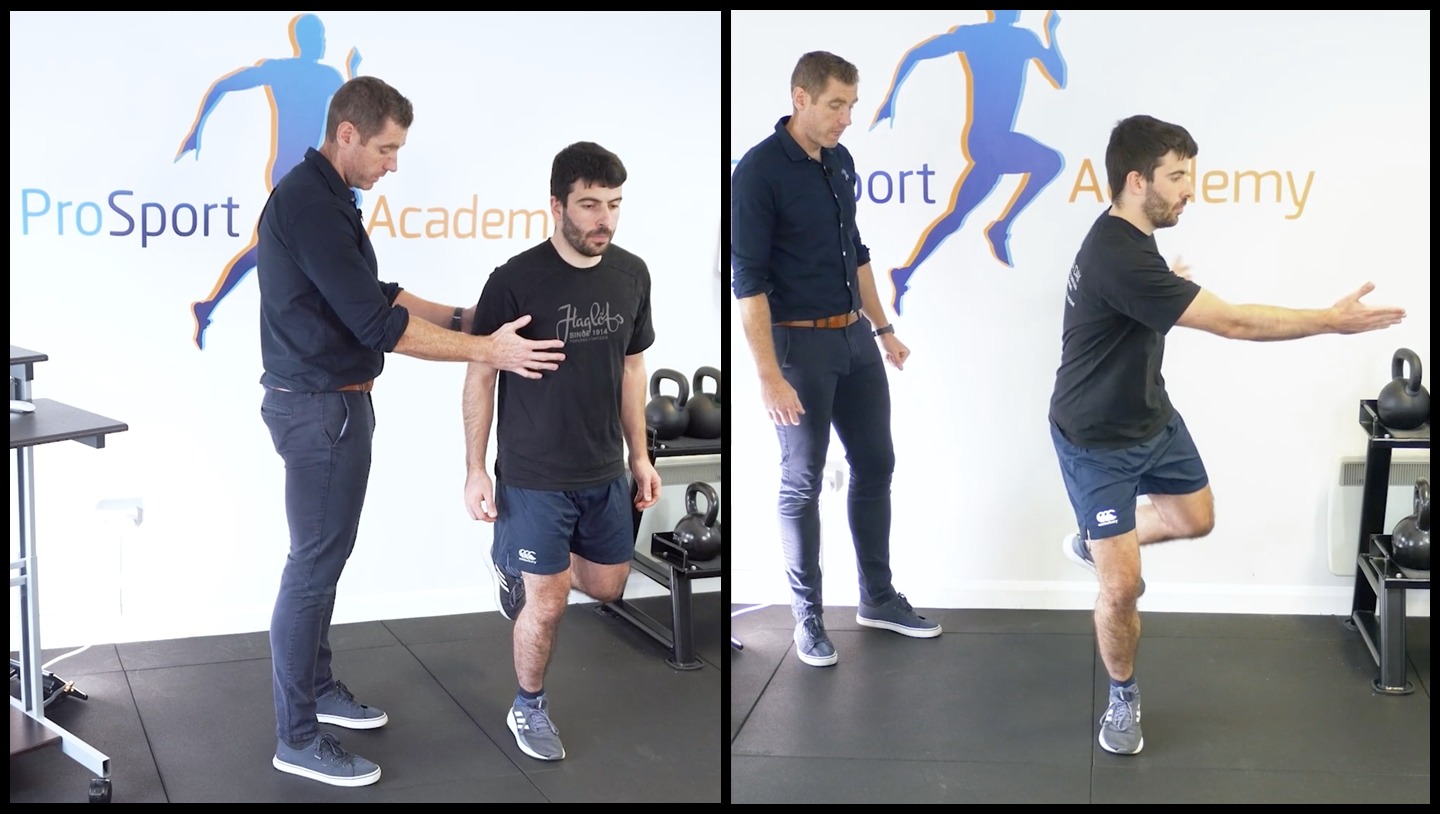
A big indicator of the severity of a hamstring injury is proximal knee flexion. Have your patient in the prone position, bring the injured leg up and attempt to bring it toward their glute whilst you provide resistance.
It’s important that you test the leg in outer range and 90 degrees to differentiate between those positions. If a patient has a good motor output at the outer range and at 90 degrees then I wouldn’t be too worried about the hamstring.
Bridging
Once you have performed the toe touch and proximal knee flexion, you’ve established that it is a hamstring issue and the ribcage and lumbar spine aren’t contributing, you need to go that one step further.
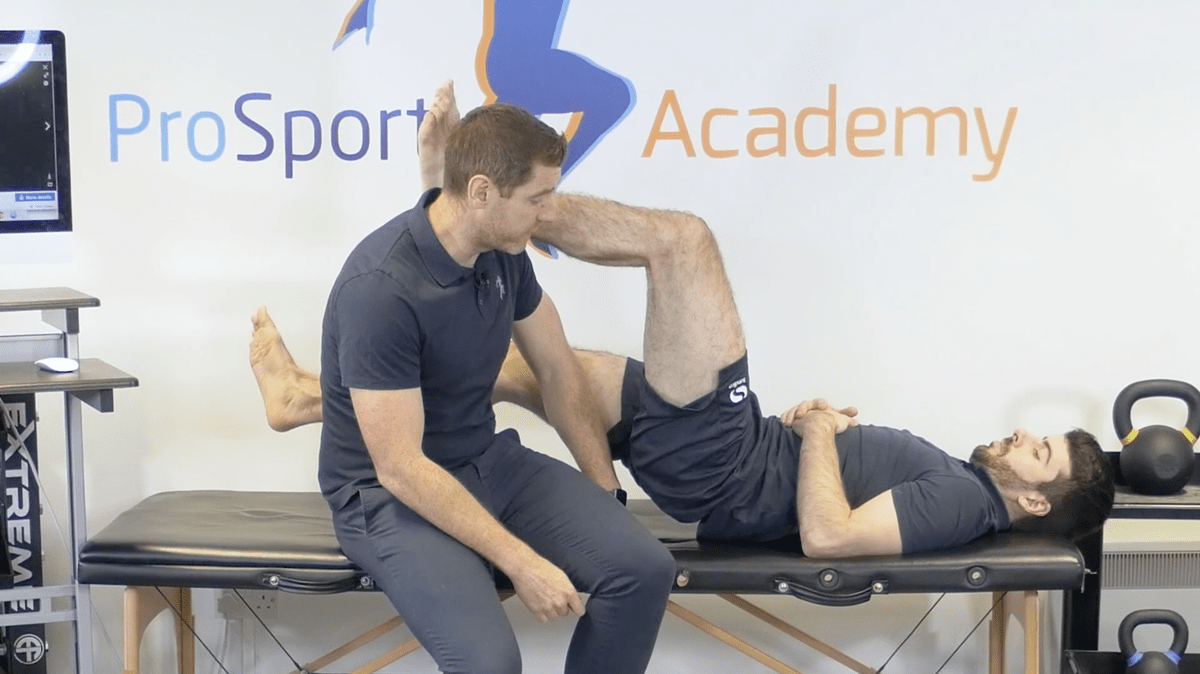
I would start by bridging with the leg at 90 degrees. You want your patient to place their heel on your shoulder, push down through the heel, and bridge up.
Then check at 45 degrees. Usually, this position will elicit pain. If they do experience pain then don’t panic, this is a chance for you to use your hands-on to desensitise those areas. After 45 degrees, test the leg higher. You want to feel the intent through their heel and feel them pushing through. If this is the case then I would say they’re happy to load the hamstrings.
The key to bridging is to be able to identify where the issue may be within the hamstring muscles. For example, if they were symptomatic bridging high up but not at 45 degrees then I would be going higher up into the proximal hamstrings to desensitise. If they are symptomatic down lower then I may want to be going into mid-muscle belly to distal.
Be very careful when you do perform this exercise. Your patients, whether they know it or not, are always looking for the simplest way to perform any exercise. Make sure they aren’t using their lower back to facilitate that movement.
But here is the key when it comes to testing. Each test is only as good as the other. Every physical therapist needs to be equipped to clinically reason, make sense of, and compare testing. For example, from my clinical experience, if a patient is happy to perform knee flexion in prone but they are struggling with the bridge position in supine I would be suspicious there is a mild hamstring issue.
If they have decreased motor output and they are apprehensive in this prone position then I would be worried that there would be some serious trauma to these tissues and would consider sending the patient for the scan to check for a more severe injury or complete rupture of the hamstring muscles.
Using These Tests As KPIs
Everyone who understands the mentorship content knows how much faith I put in key performance indicators. It’s about having the confidence and clarity to know your patient is ready to progress through your rehab. It’s about eliminating guesswork and having real evidence.
And the tests we have covered above are no different. Once you use them they then become powerful KPIs. They’re going to tell you when you can progress and when something may be going wrong. They give you a framework moving forward.
You should be looking to clear all of these. Clear the toe touch, bridging, and knee flexion at all positions. Now you’re confident of strong posterior knee stability you’re ready to move on.
Single-Leg Bridge Through The Midfoot
Before we get into your full hamstring rehabilitation program exercises we need to cover one more thing.
We have already touched on bridges but this exercise is one of the foundations to my hamstring injury rehab. In fact, I don’t just use this for hamstring strains. This is a foundation block for any lower limb injury rehab.
The reason this is so important to my rehab is because it gives me one thing… Confidence. The problem with most therapists is they are always wondering whether they can progress with their patients. Are they ready to go to standing? Are they ready to run?
But when you’re working like this then you’re only ever using guesswork. You risk your results, you risk losing those five-star reviews and referrals but more importantly, you risk your patient’s health.
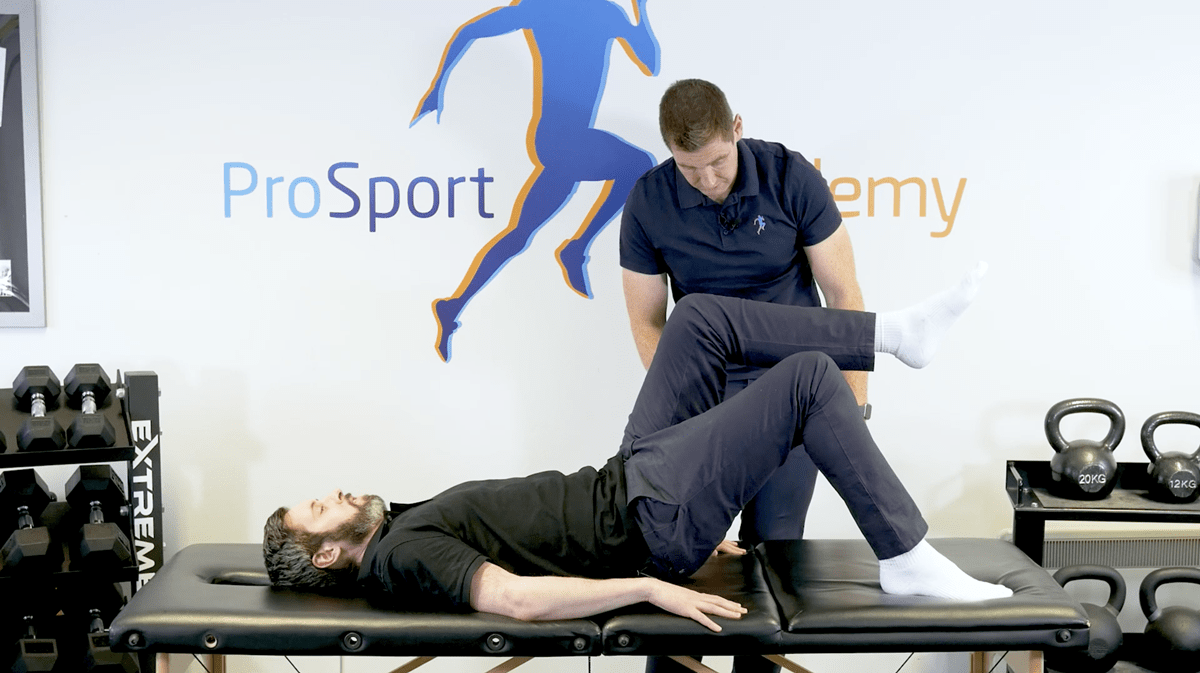
For me, including this simple single-leg bridge through the midfoot or, as I call it, hamstring load tolerance test as part of my step-by-step system eliminates that risk. Once your patient can do this without pain then you can be pretty certain they are ready to get up into standing and put more load through the hamstrings.
If you really want to understand it, you can read that HERE, but in short, you want your patient to go into the classic supine bridge position with the foot of the injured leg planted. From here you want your patient to push up through the midfoot into a plank, keeping their heel and glutes just off the bed.
When we lift the heel we are trying to shorten the gastroc. Because the gastroc and hamstrings are synergists, by shortening the gastroc we are making the hamstrings do more. We want to overload and truly test those hamstrings.
This may sound simple but I can tell you, this single-leg bridge is vital to my lower limb and hamstring injury rehab. It acts as a safety net. We are essentially overloading and causing excessive stress to those hamstring muscles.
Once you know the hamstring muscles can handle that level of loading then you know for sure that your patient can go into standing. Of course, if this motion elicits pain or your patient struggles then you know you have more work to do before you move on.
Loading The Hamstring Using A Reverse Plank
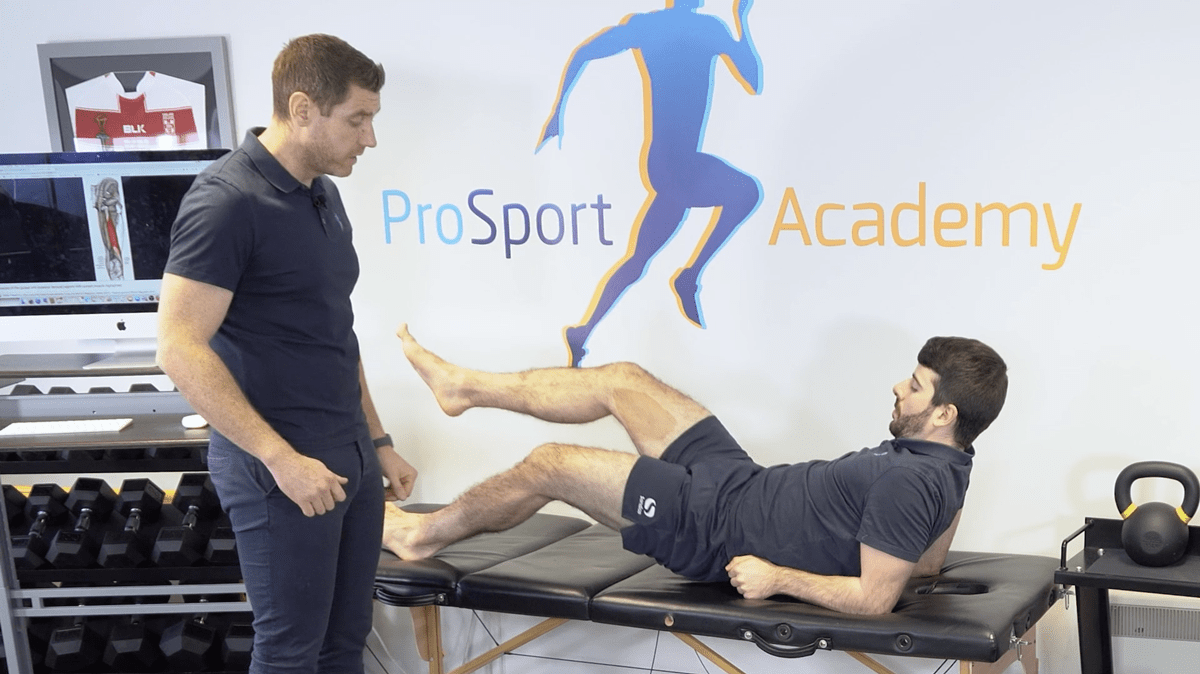
Once we have tested and established that there is a hamstring issue we want to start putting load through those muscles. Perhaps the reverse plank doesn’t fit all of our biases like midfoot pressure, but for me, it’s a great way to put a whole lot of load through the hamstring.
Have your patient start the plank using both feet planted. If this doesn’t elicit pain or any other symptoms then I would ask the patient to lift one leg off the bed. If the patient is still pain-free then this would be a good sign that we could progress a little further up your graded exposure ladder.
If you wanted to push this loading a little further then you can ask your patient to thrust and perform hip extension in this position. If they were in mild or severe pain or this plank elicited symptoms then you definitely wouldn’t want to progress them onto running.
Rehab Exercises For Your Hamstring Strain Injury
Once you know the hamstring muscles can take the level of loading needed for your patient to get into standing then it is only a case of carrying on with your step-by-step graded exposure hamstring strain rehab.
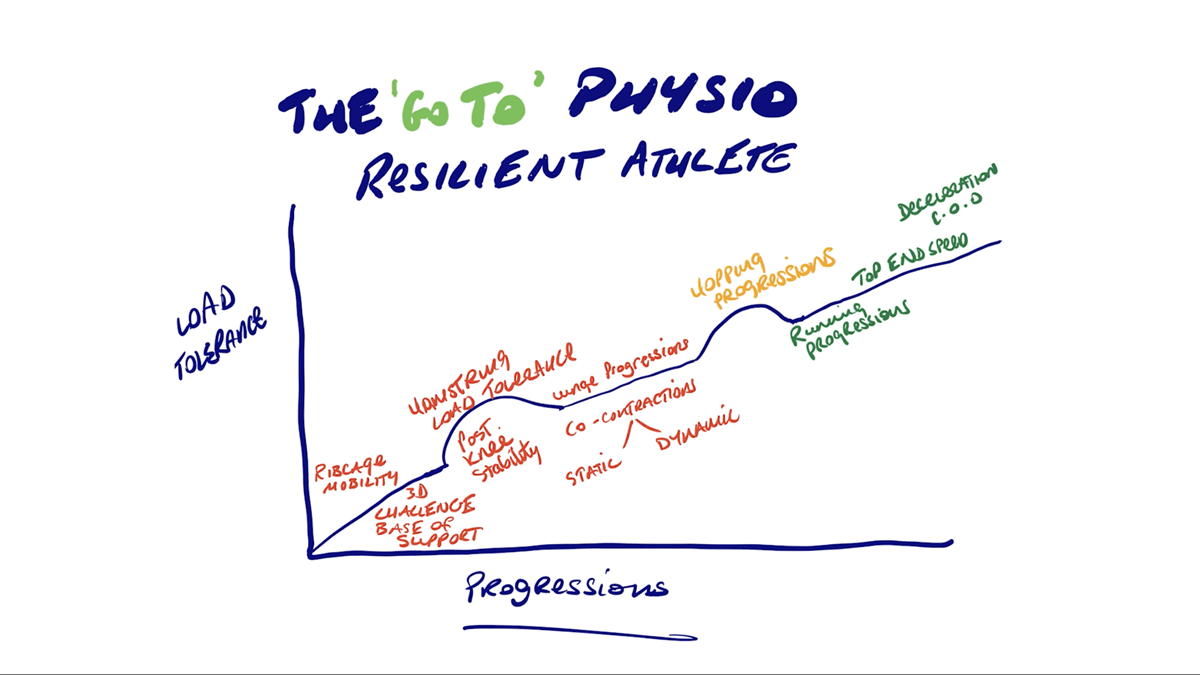
In the mentorship, we use a simple step-by-step system that is designed to take the stress and emotion out of your rehab even for a complex hamstring strain. Each progression is the next logical step.
The system allows you to truly look at your patient’s story, use the information we have gathered from the testing stage, and put together exercises to take your patient from where they are now to, as Louis Gifford put it, ‘thoughtless fearless movement’.
So what’s next?
Slouches
With these early stages, we want to start trying to get everything to work together, and slouch progressions are going to do just that. This will give your patient the ability to develop high levels of tension through the soleus and hamstrings. It will also give those muscles the chance to co-contract with the quads and allow the hip to work.
But this stage is going to help your patient find their midfoot. So many therapists skip past. They move their patient straight to hopping and decelerating and it’s a disaster. They’ll hop and stay on their heel or lean too far forward and have very few movement options. So do not miss it out.
Ask your patient to take one foot just in front of the other with a slight bend at the knee of the planted foot. Then get the belly button and chest over that midfoot.
Once they are in this starting position, you want them to relax their neck, bringing their chin to their chest putting more loads through the leg muscles. Reach down as far as they can, then cue them to squash an orange through the midfoot to come back up.
It is that simple. But like all exercises we use in physical therapy, there are a few things you have to be aware of. Firstly, you may see your patient bend their knee excessively. In this case, you really need to train that co-contraction by cueing the intent through the midfoot.
Secondly, when your patient is coming back up you don’t want their knee to kick back. If it does then the patient is just using their lower back. This is something I see if a physical therapist hasn’t used and passed their patient through the hamstring load tolerance test.
This isn’t an isolated exercise remember. It is a part of a larger roadmap to success.
Lunges
Once you have developed your patient’s ability to co-contract at the knee we want to move on to more dynamic co-contractions that will reinforce the work we have already done.
These lunge progressions give your patient the opportunity to train a co-contraction with good intent through the midfoot, we want to challenge our base of support and manage these perturbations outside of higher centre control.
Through these motions, you want to create movement with speed so your patient doesn’t have time to be able to think. We want to move away from top-down cues and toward ‘thoughtless, fearless movement’. These lunges aren’t the kind of strengthening exercises you use at the gym, we want them to build elastic energy.
You can begin simply by starting on one leg, step onto the other leg and find that midfoot without losing height. As the foot hits the floor you don’t want your patient to sink.
But the power with these exercises truly lies with you. Using these lunge exercises you can bias certain tissues with hand drivers and reaches to progress and regress, based on your assessment.
You can tailor progressions. For example, if you had a proximal hamstring strain a straight lunge would be consistent, hands above your head would be a regression because it would take load off, then leaving forward with hands outstretched would be a progression.
Understanding the reactions throughout the body and pinpointing the tissues you want to work with in the initial assessments means you have the ability to work with the lunges to bias certain tissues to address that hamstring strain.
Leaping Progressions
Once we have demonstrated co-contractions at the knee, dynamically and with speed we now need to progress to leaping.
Anyone who knows the mentorship content will know how they work as an integral part of our lower limb rehab. Just like our hamstring load tolerance test they serve as a big safety net so you can be confident and know that your patient is ready to run.
With your leaping, you want the patient to leave the floor. It may be subtle but you want enough chaos so your patient can figure it out. It can seem like a big deal to your patient but if you’re always building step-by-step then it shouldn’t be too hard.
All you will ask your patient to do is leap off one leg and onto the other. The key here is finding that midfoot and sticking on that landing leg. You should be able to give them a perturbation and they should be able to handle it.
Again you can use hand drivers and reaches to bias those tissues. for example, if you wanted to put more load through the medial hamstring then you could ask them to reach across their body.
If the patient comes back for their next session and there are no reactions then we would want to move on.
Hop And Stick
If your patient is happy with leaping then we would be looking at moving onto a hop. Your leap was from one leg to the other but the difference here is there will be more force production with your patient having to push off one leg and land on the same leg.
To begin with, we just want the patient to hop and stick. You want them to really hold that stick. If they have issues with that stick then persist for a few reps. In my experience, if you have followed your graded exposure roadmap and used the system correctly then they will figure it out quickly.
Again, you can bias certain tissues using directional reaches and hand drivers.
Hop Hop Stick
The difference with this, of course, other than the extra hop is that you really want to see the stiffness on that second hop. You don’t want your patient to sink, you want a confident movement the whole way through.
This is just the next logical step, but if you do find your patient is failing at this stage then don’t panic. Just take them back to the previous level of loading, give the brain a chance to figure it out, and come back.
Again, this is the perfect chance to use hand drivers and reaches to tailor the exercises to your patient’s problem. Just put the pieces of the puzzle together and make it work for them.
Continuous Hopping
This is the stage when your patient is going to really begin to get used to tolerating high levels of loading through the hamstring.
For this exercise, I use the hallway of the ProSport clinic but you can use any space that gives you the run your patient needs and have them hop continuously for 20 meters.
Once you have that you can build intensity, from 70% of their maximum speed to 80% and 90%. Usually, by the high-level percentages, there is a lot of load going through the tissues, they’re not sinking, they’re co-contracting well, they’re using elastic energy and that is where the confidence increases. You’re heading in the right direction.
At this point, I would send the patient away with some sets of our hop hop stick exercise and continuous hopping. When they’re back in for their next session, just recheck those KPIs to make sure there has is no pain or negative reactions.
Running Progressions
To begin your running exercises you want to start with your patient on the end line of a football field. Start your patient off running for 50 or 60 meters then walk back.
You want them to begin at 40% of their maximum speed for 3-4 reps, build up to 50, 60, and 70%. In between each of these four reps, you want to perform decelerations exercises which we will come to in just a second. This is your first session of running progressions.
When the patient or athlete comes in the next session then you can begin again. This time start at 50% of their maximum speed for 4 reps then up to 60, 70, 80, and 90%, and keep going with those deceleration drills in between.
When you have hit 90% with your patient then it is a good idea to give them a day off. Come back, start at 60%, 70, 80, 90, 100, and then what I call 110%. 110% is you giving some kind of cue and the patient having to react and sprint without thinking. In this last block, we are really looking for ‘thoughtless, fearless movement’.
The great thing about this is it is just another part of your graded exposure. You know that your patient can handle getting up to these speeds because they have been doing all of these hopping progressions.
Deceleration
With the hopping progressions, you were increasing the load, with deceleration you are bringing down that level of loading but increasing the speed of movement.
For your first stage, you want your patient to take a run-up of three steps and stick, landing on the midfoot. In this position you want them to have movement options. You want to set them up for success, whether that is taking contact in sport, sidestepping, or completely changing direction.
This is again now where your ability as a physical therapist comes into play. Use your knowledge of the patient, their issue, their injury history, put it all together, and decide what plane you’re working with use hand drivers and reaches and tailor these movements to your patient.
Treating A Hamstring Strain Injury Using A Step-By-Step System
Dealing with a hamstring strain or acute hamstring strains can be overwhelming. Trust me, I’ve been there but there is one thing that has stuck with me throughout my career…..
‘Make a mistake once and it’s a mistake. Make that mistake again and it is a choice’
This has had a huge impact on the way I work. If you can’t get the result because you weren’t prepared, if you didn’t have the confidence and clarity to do so then that is okay. It happens to all of us. But if you choose to do nothing about it and another hamstring, back pain, or knee pain case comes in, and you can’t deal with it then that is a choice.
You can throw all the hamstring stretches, muscle spindles, or exercise you like at it, but if you don’t have the confidence and clarity to take your patient from their initial assessment all the way through to ‘thoughtless, fearless movement’ then are you really going to get the result you need?
Are you building raving fans who want to tell others about the work you have done with them? Are these people going to leave five-star reviews? Are they going to help you grow a successful clinic?
Physical therapy shouldn’t be guesswork which is why, years ago, I set about designing my own system of work. As a physical therapist having the system allows you to easily progress and regress patients without second-guessing yourself at every single turn.
This isn’t just about hamstring strengthening it is about a proven system and graded exposure rehab program. It isn’t just about getting a patient pain-free it is about setting those patients up for success.
Final Thoughts On Your Hamstring Muscles Rehabilitation
In all honesty, this guide could go on forever. We could go over case studies, we could talk about single leg reaches with a step, isometric or eccentric hamstring strength exercises, Nordics, and hamstring curls, the list just goes on and on…
But if you take one thing away it should be this. If you want to achieve meaningful results with every patient, if you want the confidence and clarity to take on every complex case, if you want to take the stress and emotion out of your work and stop losing sleep over patients, then you need a system and a structure.
Through the Go-To Therapist mentorship program I have taught my simple step-by-step system to over 700 therapists worldwide. A system that has helped those 700 therapists achieve real consistent results with thousands of people in pain across the globe.
If this sounds like something you need then I want to help. Take the first step today. Just follow the link below, book a FREE 30-minute strategy call and start your journey to becoming the go-to therapist.
Get Your FREE Copy Of The Amazon #1 Bestseller That Holds The Secret To Confidently Treating Any Patient!
Download a Free ‘ebook’ copy of the 8-Step ‘World Cup’ Treatment Plan that helped my private patients achieve full recovery and made me a ‘go-to’ physio for complex cases…