If you don’t have the clarity to get your subjective assessment right then ultimately your rehab and treatment is going to be built on quicksand.
I’ve seen so many therapists stumble through their assessments, lacking confidence and missing the opportunity to set their patients up for success.
I know this because I was the same. When I think back to my assessments as a new grad, I barely recognise that therapist, body chart in hand asking any question that popped into my head. It wasn’t until I took the time to think about what these questions meant that I saw big changes in my work.
In this article, I’ll go through some of the best subjective assessment questions to set you and your patients up for success.
Keep reading to find out more.
Beginning Your Subjective Assessment
The subjective assessment or subjective examination is the crucial first step in your patient’s journey.
Whether it is shoulder pain or anterior knee pain, they have taken the steps to come to you in order to deal with their problem. You must get this right.
First impressions count.
For a therapist, this initial examination is your chance to gather information and use your clinical reasoning skills to make sense of these findings. But first, you need to know how to get this information.
With the correct questions, you can begin to create hypotheses, this will move you toward your objective assessment, using testing to source evidence leading you to a possible diagnosis, rehab, and treatment options.
Use the wrong questions and the opportunity and examination are wasted. You will ultimately reach a destination of overwhelm…
But before we get to those higher level questions there are a few special questions we should think about first.
Rule Out Red Flags
The first thing any healthcare provider should do is rule out red flags. If your patient is showing signs or symptoms that their condition could have a more serious prognosis, this needs to be addressed.
Red Flag indicators
- Constant Night Pain
- Neurological deficits
- History of trauma
- Saddle anaesthesia
- Numbness – Cauda Equina Syndrome
Most importantly, anything that doesn’t make sense from a musculoskeletal point of view could be evidence that the condition causing the pain may be worse than expected. If something doesn’t feel right with any one of your patients you must take action.
Setting Patient Expectations With A Question You Will Not Find In A Journal Article…
‘What is the most important thing you want from today’s session?’
It may seem simple, but this is always overlooked. So many therapists just don’t have the confidence to ask their patients outright what they expect from their very first visit.
This is the perfect place to start and an indicator as to where your patient wants to get to, but most importantly it will help you set expectations.
In a journal article by Hush, Cameron, and Mackey, a study conducted found that patient satisfaction is closely linked with patient expectations. This source tells us that setting and meeting patient expectations is crucial to your success as a clinician.
If a patient with chronic back pain or worsening symptoms for ten years says they want to be pain-free after session one then you must help them understand that this may not be realistic.
If there is a mismatch between what they are expecting and reality then chances are patients won’t believe you can help and ultimately they will drop off after session two or three.
In the ‘Go-To’ Physio Mentorship I teach a simple but powerful equation that can help you manage patient expectations…
If the patient’s expectation level is higher than their current reality, then their happiness level will be negative. Get patient expectations on the same level as reality and you have a patient who is positive and ready to adhere to your exercise and rehab programme.
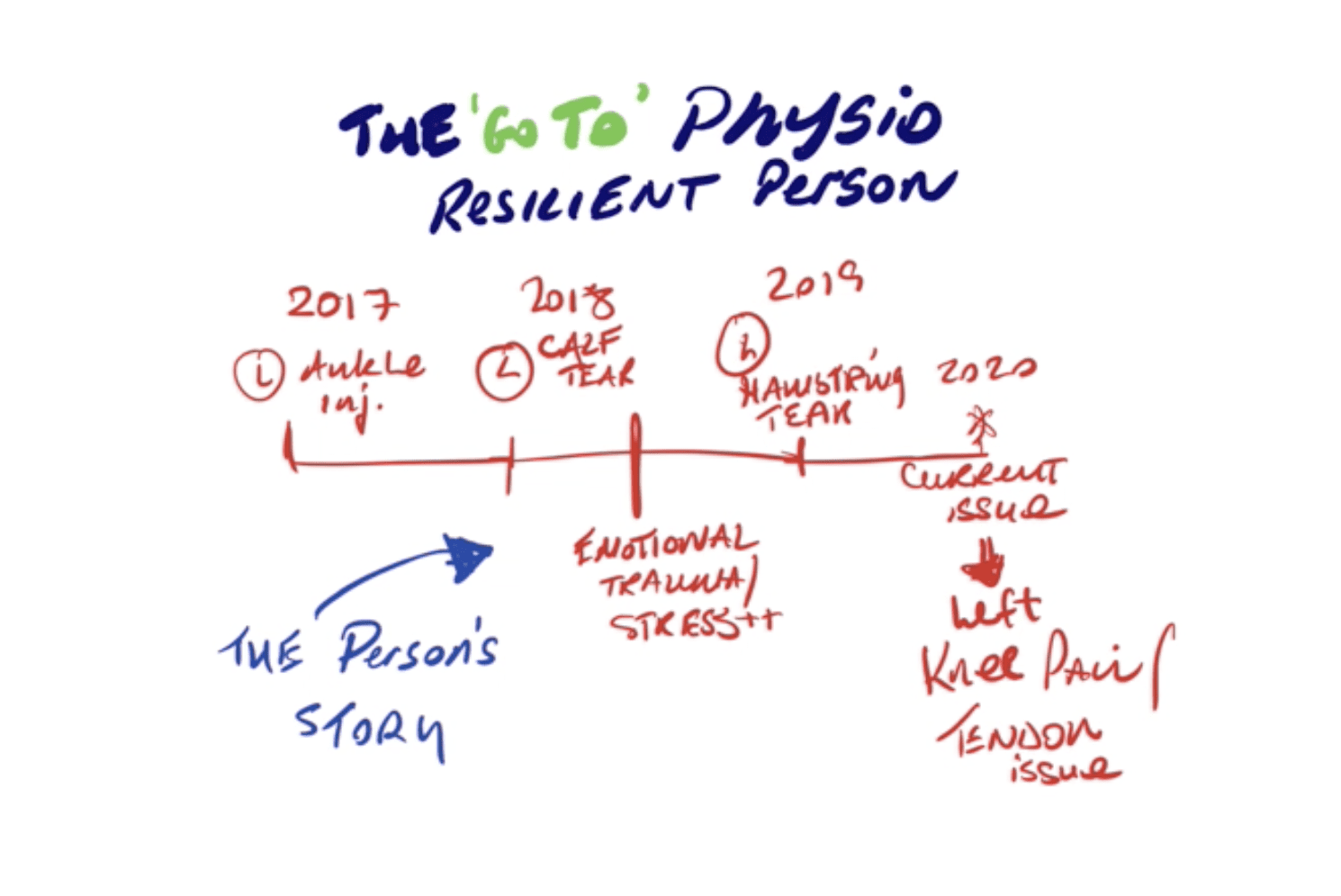
Getting Previous Injuries To Help Your Diagnosis
Ask questions and put together a clear timeline of previous injuries and stressors – Are they contributing to the pain experience?
In many cases having a clear understanding of your patient’s injury history and previous stressors will help you begin to understand why they are in pain now and what might have contributed to this issue.
Take notes on every relevant aspect of your patient’s medical history, perhaps their family history, any source of information that can lead you to a strong hypothesis and ultimately a diagnosis.
Once you have a clear picture of their injury history and medical past, begin to build around this information with higher-level questions.
Find out more about when the symptoms began, was there a specific activity that bought pain on? This will give you clues about potential muscles contributing to the symptoms.
Have they tried any medications or activity to relieve pain?
What Are The Primary Tasks The Patient Needs To Be Able To Do On A Daily Basis?
What is the pain stopping you from doing?
Whether it is back pain, anterior knee pain, or shoulder pain you need to know what primary activities these symptoms are preventing your patient from doing. This could be anything, from running to climbing the stairs.
This information is a key indicator as to where you will focus in rehab and treatment. Rather than just strengthening tissues you can focus clearly on helping that patient to succeed in life.
What Does The End Goal Look Like?
Where do you want to get back to?
You must establish your patient goals. Do they want to be able to run again or are they just interested in climbing the stairs or sleeping at night? These are key points of reference to set with your patient.
It is your job as a clinician to build a graded exposure rehab plan to meet those goals. This knowledge will help you design this plan. If your patient wants to get back to running, then you’ll know where to start with your treatment and what tissues will need to load to do this.
Final Thoughts On Your Subjective Examination
The subjective assessment is a foundational skill and at its core is the ability to ask the right questions. These are just a few to help you get the most out of every assessment. Your primary goal should be to source the information you need to improve your patient’s condition.
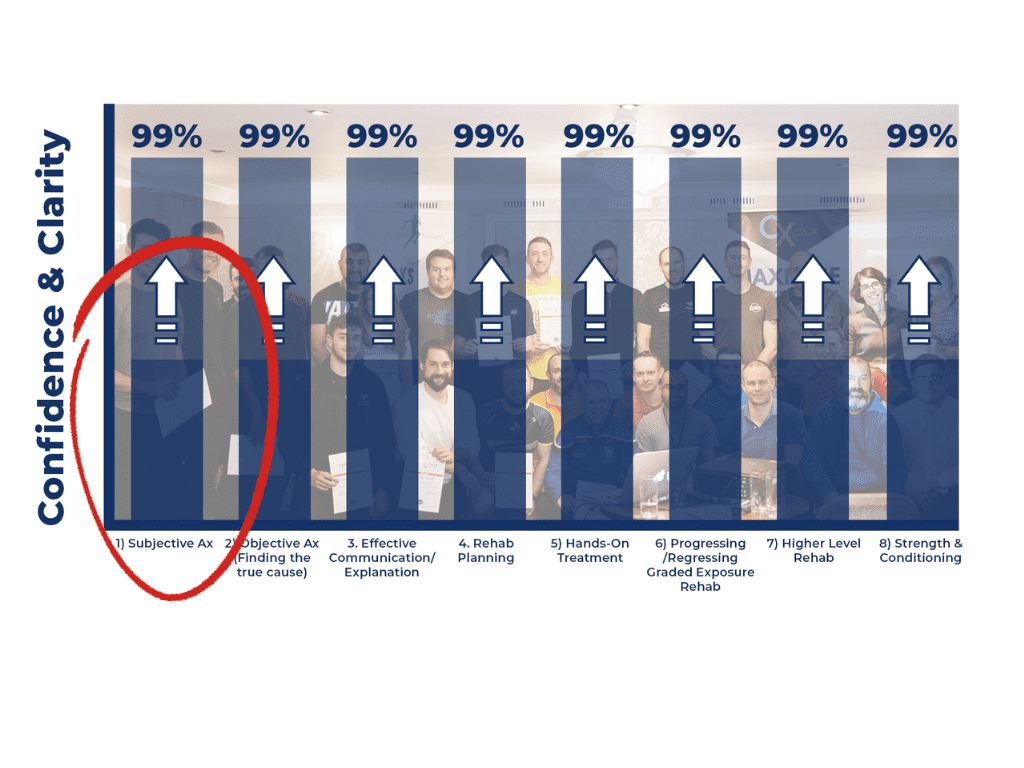
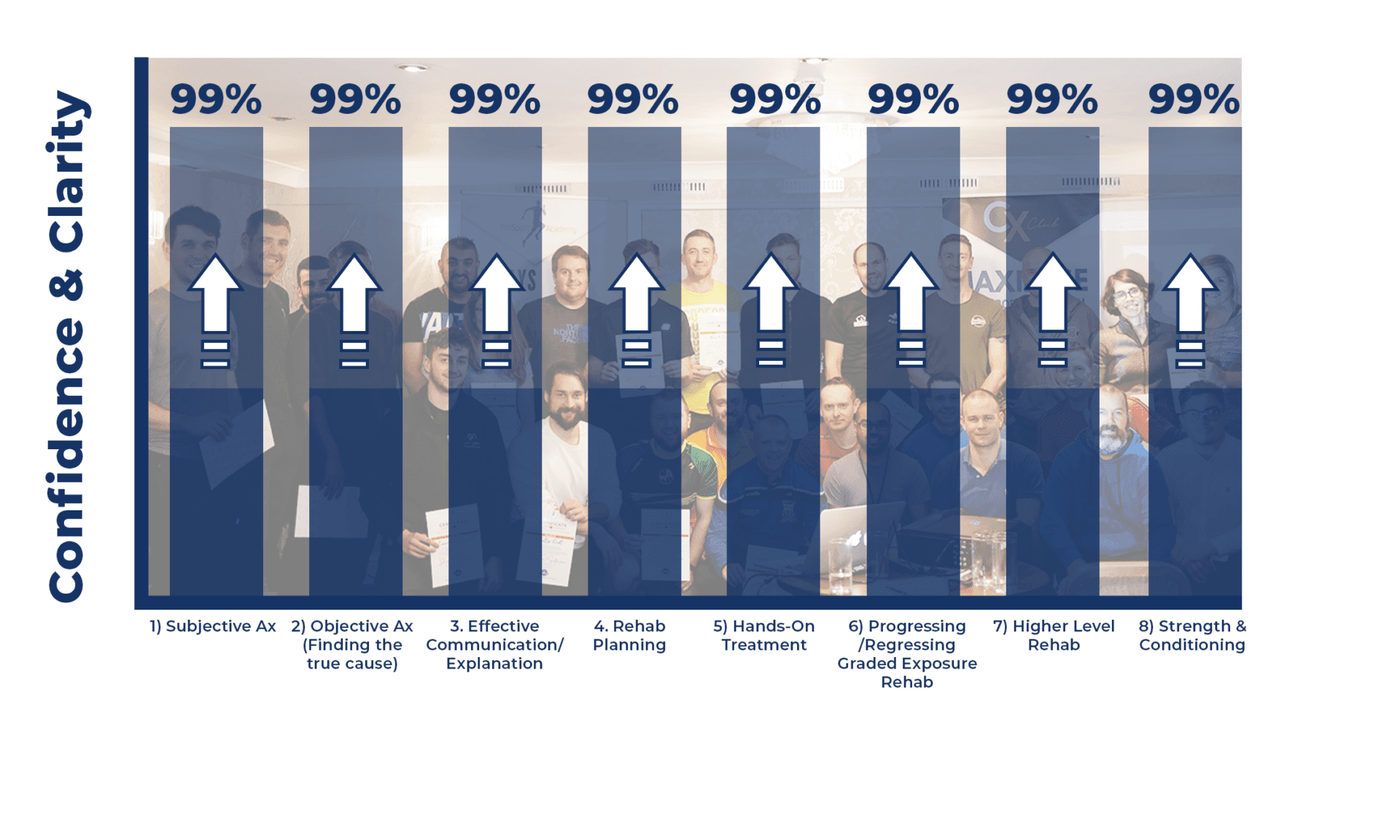
As we can see from the ‘Go-To’ Physio Pillar system, each progression in this step-by-step system is built on the last.
If you don’t have clarity in your subjective examination then you’re not putting yourself in the best position for the objective assessment, you won’t be able to provide an effective explanation, you won’t know what movements you are trying to correct with hands-on treatment, and ultimately your rehab plan is set for failure.
Remember, every question elicits an answer and every answer has clues as to what really might be going on. If you find yourself lacking clarity, go back to these simple steps;
- Rule out red flags and more serious cases – Symptoms and irritability such as saddle anaesthesia or numbness
- What is the most important thing you want from today’s session? – Set patient expectations
- Tell me about your previous injury history – Cover all aspects of relevant medical problems
- What is the pain stopping you from doing? – These can be used as references as to where you start your treatment
- What are your goals and what activity do you want to get back to? – Whether your patient wants to run or climb the stairs this will guide your graded exposure rehab programme
As we saw in the contents of the PTJ journal article, the most important thing for any healthcare provider is to set patient expectations from day one. Communicate with your patients, effectively explain, and make sure their expectations are realistic.
Remember, these questions are all part of the bigger picture. Don’t forget the information you were taught at University or learned from other CPD courses. Simply combine these with your body chart, writing notes, and all other techniques.
Are you’re still lacking confidence in the clinic? Don’t panic. Just follow the link below and gain free access to our ‘Go-To’ Physio upper limb return to play course.
You’ll learn some honest truths, but most importantly, how to get those long-lasting results with patients who have failed traditional approaches.
Get Your FREE Copy Of The Amazon #1 Bestseller That Holds The Secret To Confidently Treating Any Patient!
Download a Free ‘ebook’ copy of the 8-Step ‘World Cup’ Treatment Plan that helped my private patients achieve full recovery and made me a ‘go-to’ physio for complex cases…