SLAP lesions and repairs are some of the most divisive topics in sports medicine. But for therapists, it has an equally bad reputation. They are a real source of doubt for every therapist. Can you really help this person?
But it’s results with this kind of complex case that will form the foundation of your reputation as the go-to therapist.
For years I would take my work home with me at night. I would sit wondering if I was actually making progress. These athletes depended on me to help them back to their careers and my career depended on the results I achieved with them. It all seemed to hang in the balance.
But after seeing hundreds of complex shoulder cases and watching others treat I came to one conclusion. It will never be confusing if you have the right approach…
Today I want to save you time and effort in putting those pieces together. I want to save some of the confusion and embarrassment. I want to share with you the exact approach I use for SLAP lesion repair rehab.
Read on to find out…
- Key anatomy of the shoulder joint.
- What a SLAP lesion or tear is.
- What is a SLAP lesion repair?
- My approach to SLAP lesion repair protocol.
- A week 6 trick that may surprise you.
- A foolproof system for your SLAP repair protocol.
Key Anatomy Of The Shoulder Joint
Before we start wading into the murky waters of SLAP repair protocol we need to cover some key anatomy of your patient’s shoulder.
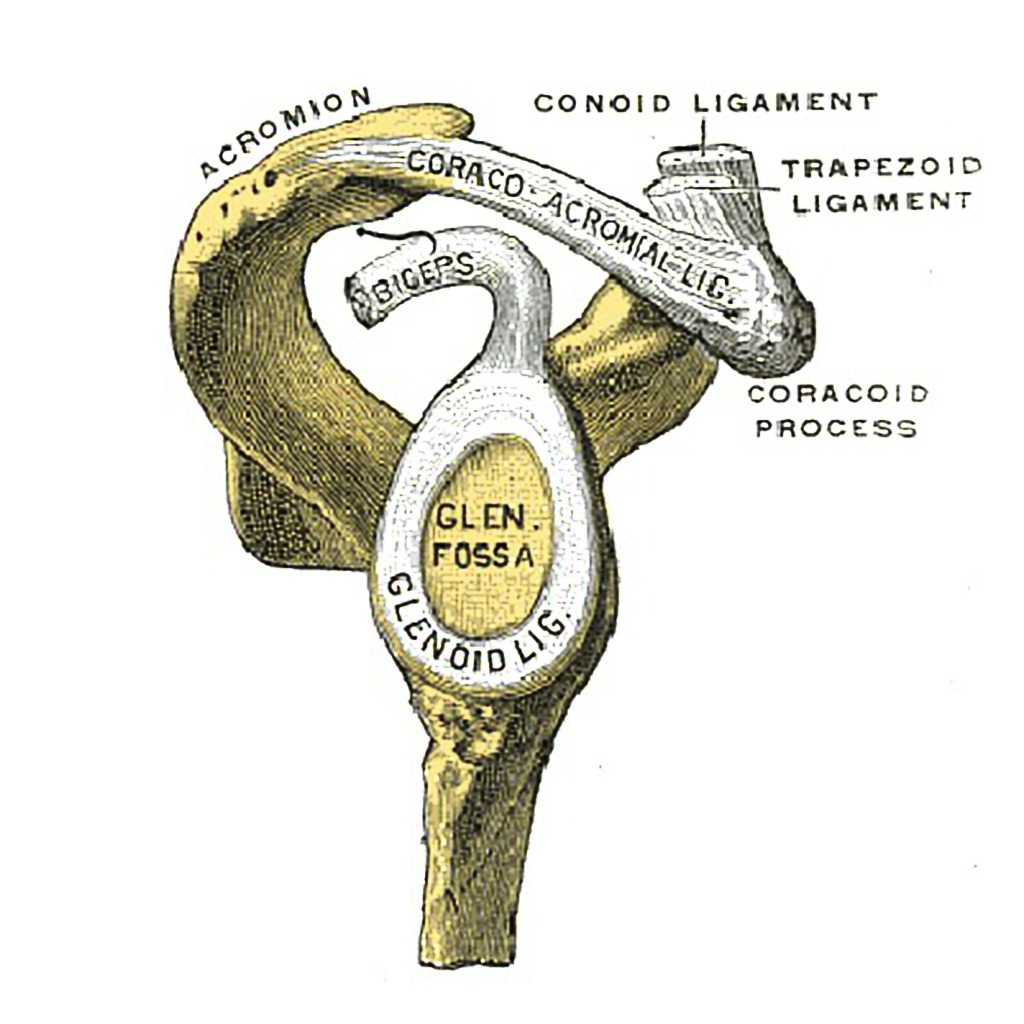
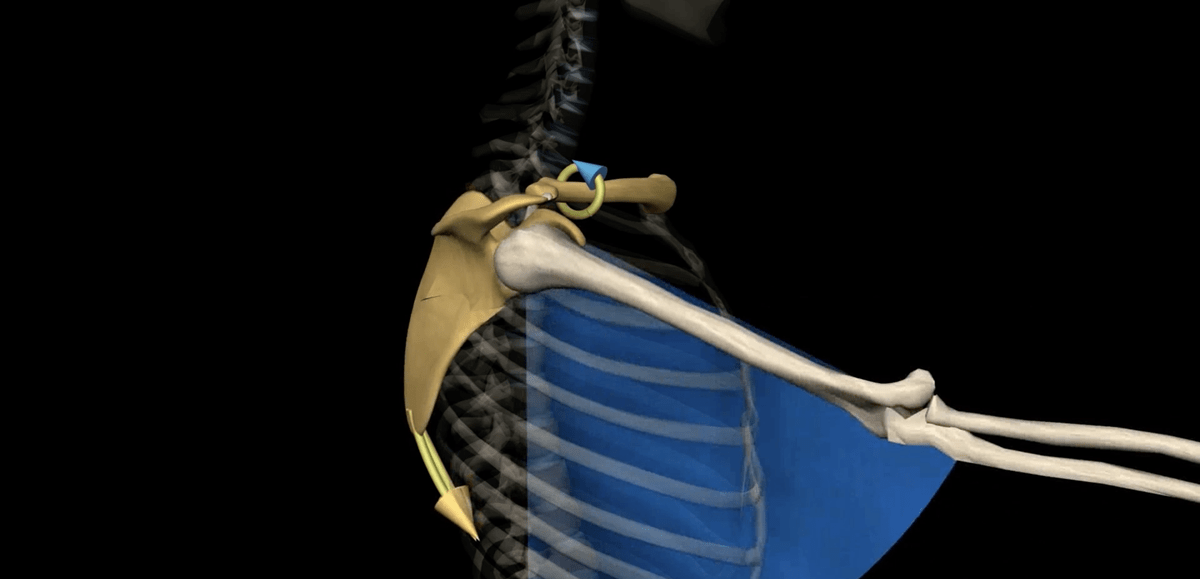
The shoulder joint or glenohumeral joint is the articulation between the head of the humerus and the glenoid cavity of the scapula. To put it simply, it’s a socket and ball joint, but dealing with this joint can be far from simple.
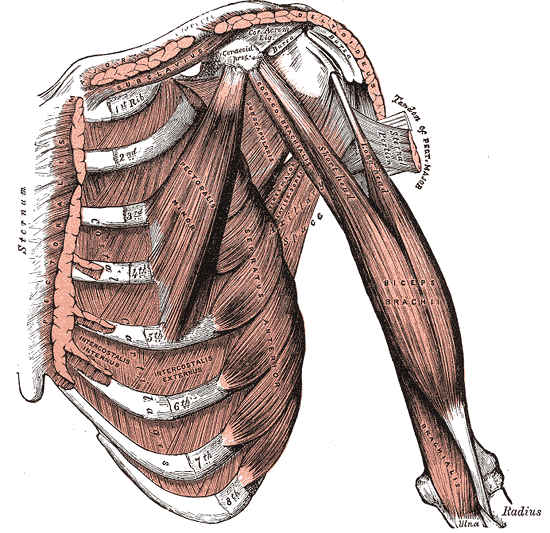
To facilitate efficient movement and increase the stability of the joint, the rim of the glenoid cavity is ringed by cartilage called the glenoid labrum. This is then surrounded by other key tissues such as the biceps tendon and various rotator cuff muscles.
All of these tissues must work together to provide your patient with a full shoulder motion, external rotation, internal rotation, and abduction.
What Is A SLAP Lesion Or Tear?
A SLAP tear or superior labrum anterior and posterior tear is essentially damage to the glenoid labrum cartilage around the socket of the scapula. This is a real pathology and causes pain and inflammation.
A tear of the labrum can be identified using a number of different tests including the O’Brien’s test and Clunk test. But for now, we are only worried about just how you can help your patient after diagnosis and repair work.
What Is A SLAP Lesion Repair?
A SLAP lesion repair is a surgical procedure designed to try and rectify the damage done to the glenoid labrum. SLAP lesions can be broken down into different categories type i, type ii, type iii or bucket handle tear, type iv all through to type x. Each type may need a slightly different repair.
Now, as a therapist, this kind of talk can be incredibly intimidating. Almost overwhelming. But it shouldn’t be.
Leave that to the surgeon. You know it’s a repair to the superior labrum and you know that person is going to need physical therapy to help them get back to the activities they need to perform in the real world.
Of course, you must pay full respect to the pathology but you must not allow this to get in the way of your real aim… Get your patients pain-free and set them up for success in the real world.
My Approach To SLAP Repair Rehab
As we teach in the Mentorship, every approach to an injury should be systematic. SLAP lesions and SLAP repairs are the same. You have to approach this in different phases.
This is where a lot of therapists stumble. They hear the word SLAP lesions followed by bucket handle tear, type ii, type iv and they feel out of their depth. Almost embarrassed to admit this is a tough case to work on. After all, we aren’t doctors.
In reality, patients don’t care what your job title is. They care if you can get them the results they need.
With passing weeks post-op you must have a solid plan and a system that will set your patient up for success in the real world.
So what are you going to do to build a successful shoulder and a successful post-operative patient?
Respect The Surgeons Protocol
Before we go any further you must be respecting the surgeon’s protocol at these very early stages from week 1 to week 3. I have sent a fair few athletes to an incredible shoulder surgeon, Len Funk. We have a great relationship and I stick by his advice whenever he gives it.
Avoid any vigorous activity to the humerus, scapula, or shoulder motion that could cause damage to that SLAP repair.
With anterior stabilization, we want to avoid any activity involving reaching out away from the body that could possibly lengthen the sutures. For posterior stabilization, reaching the hand across the body would be a bad idea.
For a surgeon, SLAP lesions can be a tricky thing to repair so you must give it the best chance of setting down and the suture anchors taking hold.
Of course, this comes first but that doesn’t mean you should stand by and do nothing…
Restoring Range Of Motion And Motor Output
When the patient does come to you and they are acute, my first call is to make an evaluation and check their arm flexion up to around 90 degrees. Here you want to get a feeling of their range of motion (ROM).
Once you have checked ROM your main focus should be on the adaptations that happen after those SLAP lesions have been repaired. The very first key performance indicator (KPI) you’re going to want to work on is restoring that ROM.
Most therapists are scared to do any damage to the shoulder and the repair of that labrum. But in the real world, if you initiate light work early on you can make some real progress.
Early Low-Level Working For SLAP Lesions
From week 1 to week 3 you can initiate light work at a low level, focussing on the biceps and triceps. You can use some hands-on treatment to reduce protective tone through the deltoid and pecs and get some ROM through elbow flexion and extension.
The great thing here is you can keep the isometrics, working at around 20-30% in that first week. Even if someone is in a sling you should be able to get that rotator cuff and the deltoid to start playing a part.
Begin by building tension through the fingertips. It doesn’t have to be groundbreaking stuff to train intent. Whether you use a table or a door for resistance, just the smallest movements and pressure can start you off.
If you can get this working in the first week post-op, then it’s real progress. You may not have that immediate strength your patient will want but if you can get those muscles, the biceps, and the rotator cuff to fire then you’re moving forward.
Of course, there are plenty more options with active-assisted exercises but in principle, you want to train through the hand, elbow co-contracted, and the shoulder. This will help stability later on.
Remember… Always work in that safe zone. If you’re not sure of what you’re doing then this is always going to be risky. You just need to begin the process of getting every tissue to do its job so you can set that shoulder up for success.
Working On All Fours
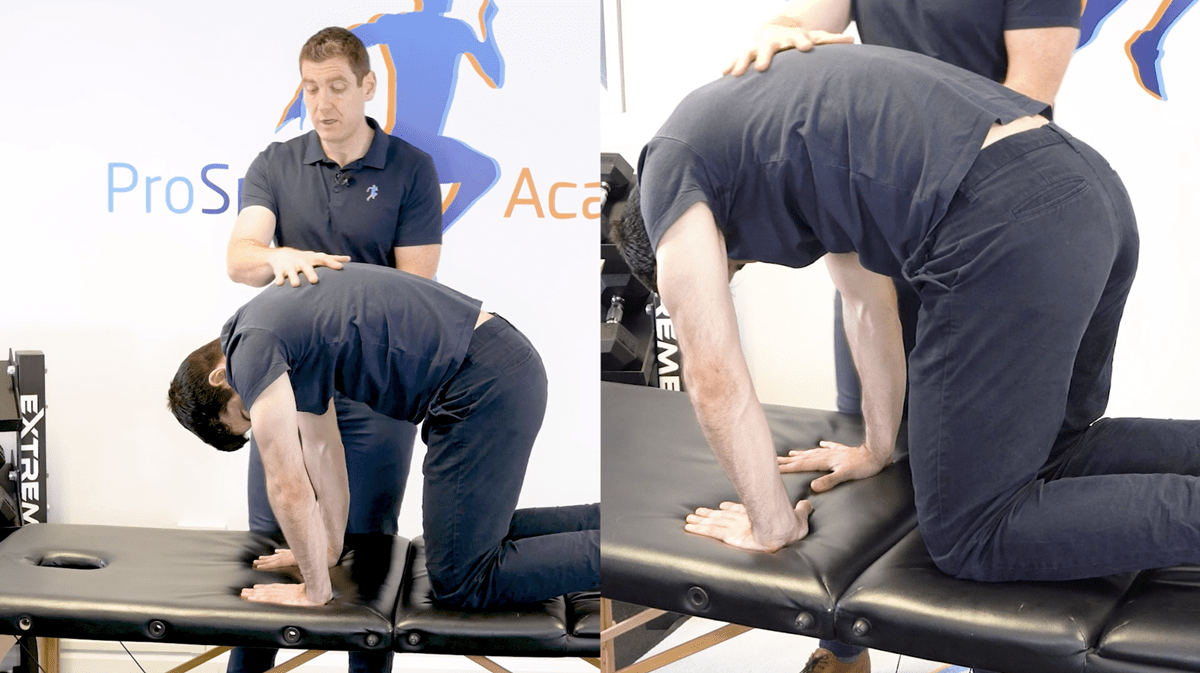
When you’re are dealing with a superior labrum anterior to posterior tear repair, once your patient is out of a sling and from around week 3, I have always found all fours work to be a great place to start.
Using these motions we are looking to restore ROM, flexion, abduction, adduction. Just remember to keep a slight bend of the elbow and real intent through that mid-hand. In this position, rock backs can be an incredibly powerful exercise but again, be careful to not push beyond the safe zones of the protocol.
Serratus Anterior Push Up For SLAP Lesion Repair Rehabilitation
An incredibly powerful variation to your all four work is a serratus anterior push-up. With your patient on all fours, you want them to arch their back, you want the ribcage to come up and retract through the exhalation.
But rather than actively pushing we want the exhalation to do that. Breathe in through the nose and exhale until the ribs come up. If you can get the ribcage down and retracted then you’ll have the serratus anterior working with the internal obliques and this whole process will help set that glenohumeral joint up for success.
Using Your Upper Limb Return To Play For Your Superior Labral Tear Repair
Once you have range of motion you want good motor output in all four directions, through the anterior, posterior, medial, and lateral. Following that you can move on to build load tolerance on all fours and then press-ups.
This should be up to around week 6. This timescale may differ from patient to patient but it is up to you as the therapist to have the confidence and clarity to know these progressions are right.
Now the next step is simple. You hit week six and you just roll into your upper limb return to play. Your gradual progressions should have worked so you know your patient is ready to move up.
Using A System For Your Superior Labrum Anterior Posterior Tear Repair
As therapists, we find it so easy to get lost in our heads. And believe me, I was the same for years. I’d have an athlete with a type ii or type iv superior labrum repair and I’d lose focus. I’d be aware that the patient knew I wasn’t confident.
In reality, it just takes a few simple steps and a system to bring it back down to the basics so you can get the results your patient needs and you deserve.
So here it is…
In the first three weeks…
- Respect the surgeon’s protocol and remember your stabilization. Let the repair heal!
- Restore Range of motion – biceps and triceps low level – through flexion and extension and hands-on – getting tissues to fire depending on the safe zone.
- Keep isometrics in these early stages using the fingertips.
Once they’re out of a sling at around week 3…
- Use all fours to restore flexion, abduction, and adduction. Use rock backs and keep building tension through the fingertips.
- Use some active-assisted if that is what you’re used to but any movement that uses the hand, elbow co-contracted, and the shoulder.
- Once you have full ROM you want a good motor output through all four directions. Build load tolerance in all fours and with press-ups.
Once you have these then you can just feed it into your upper limb return to play.
Final Thoughts On Your SLAP Repair Protocol
I’d be lying if I said SLAP repair protocol can’t be intimidating. Of course, it can. But it doesn’t have to be complicated.
It’s all about your approach. Throughout my 13 years experience in professional sport and private practice there is one thing that has saved me time and money. It has got me real long-lasting results and has saved me the embarrassment that comes with complex cases.
It’s a simple system. Whether it is a type ii or type iv SLAP tear, a hamstring injury, or back pain, there really should be no difference in your approach. You must have the confidence and clarity to deal with any patient and you must understand the WHY behind everything you do. If you can take the stress and emotion out of it all then you can truly bridge the gap with every single patient.
Your rehab isn’t a sprint and it isn’t an endurance race. Just a set of logical steps to build successful patients.
If you’re looking for the most simple and direct path to creating world-class treatment plans that don’t just focus on the symptoms but allow you to find and address the true cause… If you want to know that every patient will turn up for every session and secure their adherence to your rehab…
Click the link below and book your FREE 30-minute no-obligation strategy call today.
Get Your FREE Copy Of The Amazon #1 Bestseller That Holds The Secret To Confidently Treating Any Patient!
Download a Free ‘ebook’ copy of the 8-Step ‘World Cup’ Treatment Plan that helped my private patients achieve full recovery and made me a ‘go-to’ physio for complex cases…