From the hundreds of clinicians I’ve spoken to, this seems to be the most overlooked part of a therapist’s arsenal in quickly improving their confidence and clarity.
Non-Negotiable Subjective Assessment Questions To Consider For Back Pain And Serious Pathology
Before we cover simple ways to instantly improve your subjective assessment, it needs to be said you cannot overlook what you have been taught in your university training. The below tips do not replace your foundational skills but rather add to them.
Key Elements Of Your Subjective Assessment
A subjective assessment is used to search for key information and review a patient’s condition, pain, and general health history. It’s a starting point at which you begin to understand a patient’s body.
Well executed, the subjective assessment is a powerful clinical tool. The right questions and a full review of your patients’ signs and symptoms will lead you to a strong hypothesis on what is really going on.
Following the assessment, the information gathered, coupled with your clinical reasoning skills will act as a guide through your objective assessment, physical examination, and any other tests you use. The subjective assessment is your first crucial step towards a diagnosis and treatment.
In short, it’s the very beginning of your patient’s journey.
Body Chart
This form will allow you to position and pinpoint pain based on the information your patient is providing.
Locate the position of the pain.
Note if the pain shifts or moves
Aside from pain are there any other symptoms or sensations?
Help patients to estimate the level of pain.
Aggravating Factors
Find out when symptoms are present and if they link to activity or time of day.
Consider when pain occurs.
Note the factors that cause the onset of pain.
Are symptoms restricted to, or worsened during certain times of the day?
Activities that may cause pain or symptoms to worsen, perhaps through work or exercise.
Easing Factors
Note when your patient finds relief from symptoms. As well as contributing towards your hypothesis and diagnosis, the signs here can often be a general indicator for what treatment may improve your patient’s condition.
Note when the pain eases.
Are easing symptoms linked to a certain time of day?
Activities that may impact symptoms in a positive way.
Current History
This should be a thorough history of the condition from the time it began to now.
Treatment since symptoms began.
The events or activities that your patient believes may have caused the injury.
Has pain worsened over time?
Past Medical History
You want a key picture of your patient’s general health over the years and whether previous conditions could be associated. It’s also important to note that family history may also play a role.
Have these pain or symptoms occurred in the past?
Note a past injury or condition that could be associated i.e. arthritis or related pain.
Have they attended therapy or received treatment before?
Related conditions present in close family members.
Social History
Gathering information on your patient’s social history is just as important as their symptoms. So many contributing factors are related to lifestyle.
Employment – effect of symptoms on their ability to work, work pattern, day/night shifts.
Relationships – children, partners, do they provide full-time care?
General activities including exercise.
Stress levels due to lifestyle.
Unfortunately, common sense isn’t so common so please ensure you rule out any red flags such as
Cancer – an unexplained weight loss of > 5kg in 1 month, constant pain
CNS pathology – loss of sensation and strength in arms/legs
Cauda Equina – weakness and/or numbness in both legs or groin area and loss of control with bladder
Fractures – night pain, recent mechanism of trauma
Infections – fever, night sweats, generally feeling unwell
Among others…
Now that we’ve covered those, let me show you how to instantly improve your subjective assessment…
The Beginning Of The Subjective Examination Is Critical
Person First, Physio Second
Therapists often overlook the fact that when we meet a patient for the first time, they are very nervous and even skeptical of us. The first impression is very important and we need to be able to communicate on a person-to-person level first and foremost.
Patients need to be able to relax and feel somewhat comfortable in our presence so they can ACTIVELY LISTEN to our questions, be comfortable enough to think about them, and give you honest answers as opposed to just blurting out the first thing that comes to their mind (Think of a job interview when you were nervous and just say the first thing that comes to your mind).
This will help you understand the patient’s story in much more detail and help encourage them to be forthcoming with important sensitive information such as pelvic floor problems, which may or may not be a clue as to what is potentially contributing toward a patient’s back pain for example.
Asking patients sensitive questions in the first five minutes of meeting them is like going on a first date and asking the person to marry you after a few minutes! You need to build trust first and foremost. Start with some easy questions so the patient is comfortable listening to you, able to process the information, and respond in an appropriate manner.
“Asking a patient some sensitive questions in the first five minutes of meeting them is like going on a first date and asking the person to marry you after a few minutes!”
What are the consequences of not doing this?
Well, firstly, are they really understanding your questions and giving you accurate answers?
And second, if they are still skeptical and nervous and you move onto the objective assessment, what influence will this have on their movement strategies?
I remember when I entered a course late one day, I was feeling rather nervous and was consciously aware of people’s eyes whom I did not know looking at me as I took my seat. I remember my muscular tone had changed, I was tense and even felt awkward walking. Can you remember a time like this? What impact will this have on your objective assessment with how a person REALLY carries themselves in real life versus how they are moving now?
Are you willing to label this movement as ‘dysfunctional’ and design a treatment and rehab plan on this objective assessment or pillar 2 alone?
Or in regards to pillar 5 and interventions… you are explaining what pain is and is not to a patient. If the patient is still nervous and even skeptical, you’ll probably find this type of patient nodding their head away in agreement, yet you know they are not actually processing the information. They are not really listening to you. Has this ever happened to you?
Is this the patient’s fault or is it the therapist’s fault? Just food for some thought…
I hope you can now see the importance of making patients feel comfortable in your presence from the very first minute. If you get inaccurate results in your objective assessment or the patient ‘just didn’t get it’ when you were explaining pain to them, where was the initial problem?
I would argue it was right back in the first 60-180 seconds of meeting the patient…
An Opportunity To Let Them Know What Is About To Happen
A big issue for a lot of people is the fear of the unknown.
The subjective is a great opportunity for you to explain exactly what is about to happen in the session ahead but also the weeks ahead.
This also serves as a great opportunity for you to establish authority in the relationship and help the patient have confidence in you.
Patients believing you can help them and having trust and confidence in you is half the battle. This starts in the first 60-90 seconds.
You can invest thousands and thousands of pounds on the latest hands-on treatment courses but if the patient does not believe deep down that you can help them, then these techniques may be of limited value.
Again, appreciate the power of pillar 1 to set the tone (in a friendly manner) for the session ahead but also an opportunity for you to instill confidence in the patient that they have made the right decision in choosing you and there is a clear path to follow to get them back to living their life pain-free.
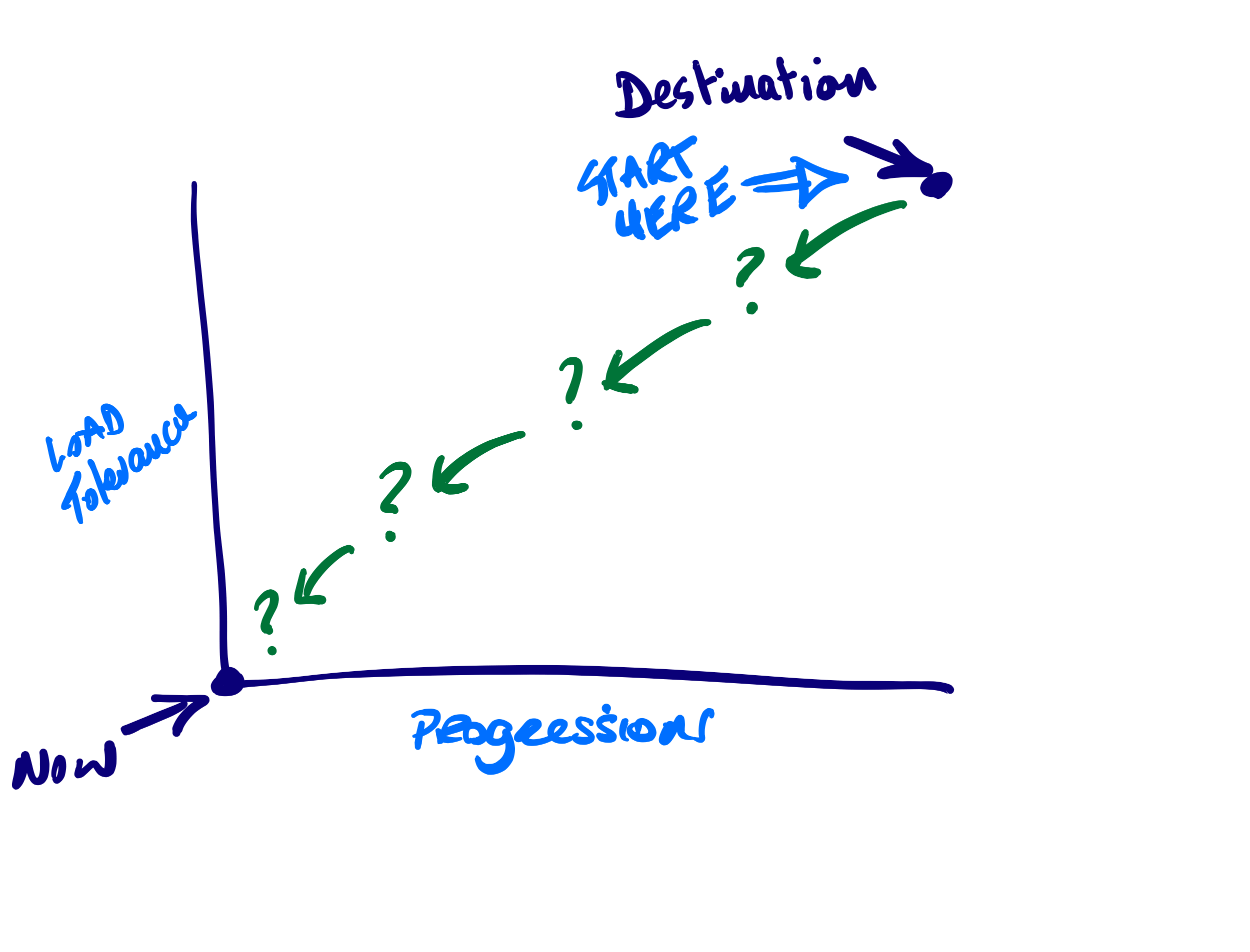
Where They Are Now And Where They Want To Get To
One of the biggest mistakes I made early in my career in professional sport was assuming that the athlete knew what was going to happen over the coming months.
For example, they have just suffered a Grade 2 MCL or an ACL. Someone (maybe even you) will have told them it’s a 6 week or 6-month injury and most athletes will accept that.
But for a lot of athletes, the fear of the unknown can be a major block to getting back. They almost assume that in 6 months’ time they will wake up one morning and feel great and get back to training.
Taking the fear of the unknown away, giving the athlete a clear plan and understanding of what is involved is invaluable in helping them to be crystal clear on where they are going.
This serves two purposes, it allows the reticular activating system to selectively tune their attention into helpful things but also stops them from focusing on the injury or negative aspects of the injury.
Think of a persistent pain patient…
And you ask them what they want. Most will say something along the lines of ‘I just don’t want this pain anymore’…
But the problem is most patients are very good at knowing what they DON’T want but actually have no idea of what they DO want, and what that actually looks like.
And until you know this, how can you effectively create a bespoke treatment or rehab plan for them?
Again, food for some thought…
The problem is most patients are very good at knowing what they DON’T want but actually have no idea of what they DO want, and what that actually looks like so how can you design a treatment plan using pillar 4?
In The ProSport Academy ‘Go-To’ Therapist Mentorship, I teach a nice drill to extract this information. I learned it from one of the world’s top sports psychologist’s Karl Morris and hand’s down, spending the first session identifying what the patient actually does want have improved my results tenfold over the last 4 years.
I would encourage you to be crystal clear on what the patient wants before you even worry about putting an exercise on paper.
Get Your FREE Copy Of The Amazon #1 Bestseller That Holds The Secret To Confidently Treating Any Patient!
Download a Free ‘ebook’ copy of the 8-Step ‘World Cup’ Treatment Plan that helped my private patients achieve full recovery and made me a ‘go-to’ physio for complex cases…